MTA-SZTE Dermatological Research Group
Principal investigator: Prof Lajos Kemény, MD, DSC
Investigations on the interaction of the cutaneous microbiota and skin cells
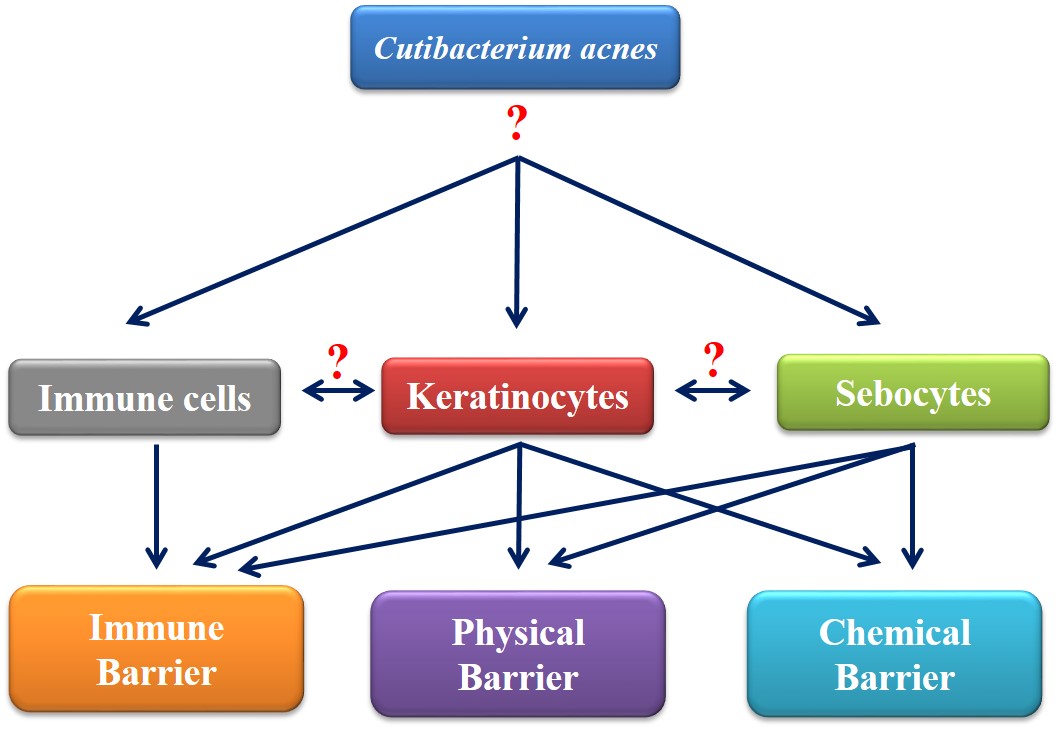
The human skin is an important gatekeepers of our body, forming a complex barrier. It distinguishes between friendly microbes and harmful invaders and initiate effective immune responses if necessary. Our skin harbors a specialized microbial flora, which plays a crucial role in the maintenance of the epidermal homeostasis, but it can also contribute to the pathogenesis of different skin diseases. A prominent member of this community is Cutibacterium acnes (C. acnes, formerly known as Propionobacterium acnes – P. acnes) is a dominant microbe especially in sebum rich skin regions from puberty. Even though this bacterium is commonly found in healthy skin, it may also initiate innate immune- and inflammatory reactions in epidermal keratinocytes leading to the formation of characteristic inflammatory acne lesions.
Our workgroup is aiming to characterize the complex interaction that exists between skin cells and C. acnes bacterium.
One of the most important function of the skin is forming an immune barrier. Tight regulation of induced innate immune activation in skin cells is crucial, as these processes may turn deleterious if not properly controlled. We identified two possible factors (TNIP1, TNFAIP3), as potent negative regulators of C. acnes-induced TLR signaling pathways. All trans retinoid acid (ATRA), an effective drug used for acne treatment can modify TNIP1 mRNA and protein levels, and through that modulates proinflammatory cytokine and chemokine expression. Our results suggest that TNIP1, TNFAIP3 may play important roles in limiting the rate of immune activation and subsequent inflammation in keratinocytes, helping to maintain skin homeostasis.
Another important function of our skin is to form a physical barrier. Based on the results of in vitro cell and organ culture studies we propose that C. acnes can also modulate the barrier properties of our skin, which may be a result of expression and localization changes of certain proteins (e.g., CLDN1, CLDN4, OCL, ZO-1) forming specialized cell to cell contacts called tight junctions.
Together with the available data from the literature our results may enhance our understanding of the properties and functions of the cutaneous microbiota in healthy skin and under pathogenic conditions.

